Dogma — prescribed doctrine proclaimed as unquestionably true by a particular group — a settled or established opinion, belief, or principle.
In 2021, research concluded that medical orthodoxy, such as ‘droplet dogmatism’, blocked the acceptance that the SARS-CoV-2 virus was mainly transmitted through the air, in spite of knowledge from fields outside infectious disease.
Three fields—political, state (policy and regulatory), and scientific—were particularly relevant to our analysis. Political and policy actors at international, national, and regional level aligned—predominantly though not invariably—with medical scientific orthodoxy which promoted the droplet theory of transmission and considered aerosol transmission unproven or of doubtful relevance. This dominant scientific sub-field centred around the clinical discipline of infectious disease control, in which leading actors were hospital clinicians aligned with the evidence-based medicine movement. Aerosol scientists—typically, chemists, and engineers—representing the heterodoxy were systematically excluded from key decision-making networks and committees. Dominant discourses defined these scientists’ ideas and methodologies as weak, their empirical findings as untrustworthy or insignificant, and their contributions to debate as unhelpful.
Conclusion:
The hegemonic grip of medical infection control discourse remains strong. Exit from the pandemic depends on science and policy finding a way to renegotiate what Bourdieu called the ‘rules of the scientific game’—what counts as evidence, quality, and rigour. —Orthodoxy, illusio, and playing the scientific game
Last week new research was published, confirming that dogmatism within scientific boundaries resulted in further spreading the virus, in spite of knowledge of how to mitigate spread.
One may say that the delay was only 3 months; perhaps that is only a short interval considering that we are now in the third year of the pandemic. However, those early 3 months were critical, because this was when control measures were being developed and introduced in countries around the world. This was also the time when public interest was most acute and messages around transmission were embedded into the actions that millions of people took in their daily lives. The “hygiene theatre” (as it was later called) was established, and for at least the next 12 months, hands were disinfected countless times during the day; surfaces in public spaces were deep cleaned; groceries from supermarkets were disinfected; and gloves were worn to avoid surface virus. But the virus was principally in the air, with even now limited evidence that fomites or hard surfaces play a significant role in transmission. The initial misguidance and subsequent mixed messages have delayed practical implications from being implemented as vigorously as they should have been, from recognizing the importance of airborne transmission to implementing controls demonstrated to be effective. Two and a half years later, in November 2022, the then WHO Chief Scientist admitted: “We should have done it much earlier [calling SARS-CoV-2 airborne], based on the available evidence, and it is something that has cost the organization.” —COVID-19 and Airborne Transmission: Science Rejected, Lives Lost. Can Society Do Better?
Back in 2006 I had asked — who are the experts? — specifically that it is getting difficult for anyone to be an expert other than in a very narrow field for a short period of time. I noted that hierarchies and experts have a symbiotic relationship. Without hierarchies, no authority can tell us who is the expert. I asked, tongue in cheek, if humans were able to learn before there were hierarchies and experts. Today, it is becoming evident that experts can be the source of a problem instead of its solution.
Established and institutionalized professional organizations too often lack the diversity of thinking necessary to deal with complex problems, such as a novel coronavirus.
“As we are becoming more entangled with our technologies, we are also becoming more entangled with each other. The power (physical, political, and social) has shifted from comprehensible hierarchies to less-intelligible networks. We can no longer understand how the world works by breaking it down into loosely-connected parts that reflect the hierarchy of physical space or deliberate design. Instead, we must watch the flows of information, ideas, energy, and matter that connect us, and the networks of communication, trust, and distribution that enable these flows.”—The Enlightenment is Dead, Long Live the Entanglement
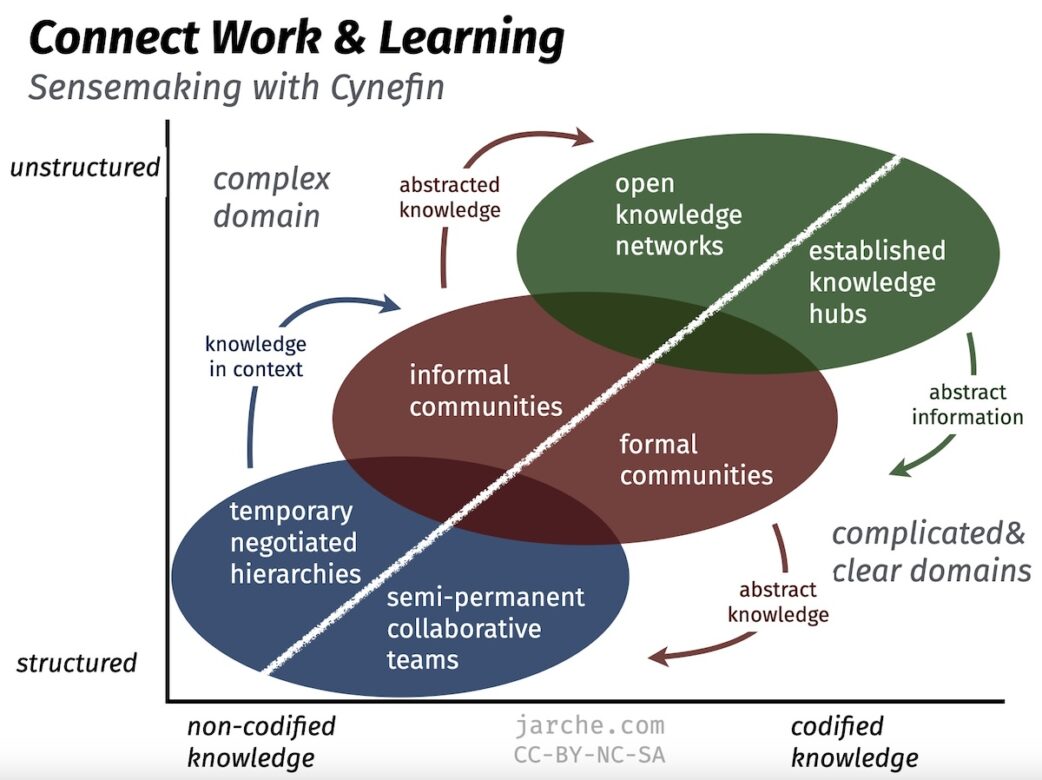 In navigating complexity we cannot rely on thinking and organizing for ordered domains. There are — at least — two modes for each organizational form (teams, communities, networks) required to work and especially learn. For example:
In navigating complexity we cannot rely on thinking and organizing for ordered domains. There are — at least — two modes for each organizational form (teams, communities, networks) required to work and especially learn. For example:
- Teams can be semi-permanent and collaborative in ordered domains but should be quicker-forming temporary negotiated hierarchies in the complex domain.
- Formal communities can provide continuity in ordered domains but informal communities are needed to provide more flexibility in crossing expertise silos and disciplines.
- Established knowledge hubs provide all the structured information that a discipline requires, like the Project Management Body of Knowledge, but open knowledge networks are better when facing the complexity of the SARS-CoV-2 pandemic as they need to quickly incorporate new findings and knowledge.
In the case of infectious disease prevention and public health, the established knowledge hub of the WHO was inadequate for sensemaking in the complex domain. These professional bodies need to develop ways to effectively connect with more diverse and open knowledge networks. The digital networks that now connect all of us globally can give us a new sense-making platform that many of us and most of our leaders ignore or use inappropriately.
Leadership today is helping make the network smarter, stronger, and more resilient. One person cannot lead in a connected world. One profession cannot make sense of complex situations alone. If they try, they become the knowledge bottleneck, as shown by the influential ‘droplet dogmatics’ at the WHO, CDC, and elsewhere.
